In 2015, the American College of Obstetricians and Gynecologists suggested we should view the menstrual cycle as a vital sign.
Menstrual health is directly related to a woman’s overall health and systemic function, making it just as important as one’s heart beat, blood pressure, body temperature, and respiratory rate!
Are you are a practitioner looking to support your female clients in their hormone-balancing and cycle-healing journeys? This article will teach you the basics of how to achieve an inside look on a women’s health through using the menstrual cycle as a vital sign and diagnostic tool.
What is The Menstrual Cycle?
First, we have to understand that the menstrual cycle and menstruation are two entirely separate things.
The Menstrual Cycle:
The menstrual cycle is an average 28-day process that begins with the first day of a woman’s period and ends the day before her next period. The menstrual cycle can be broken up into 4 distinct phases, each consisting of different metabolic processes. These phases are the follicular phase, ovulatory phase, luteal phase, and menstrual phase. The hormonal fluctuations that influence each of these phases are what make up the menstrual cycle.
Menstruation:
At the end of the month, the steroid hormone, progesterone, drops to its lowest point. This triggers the release of inflammatory prostaglandins. These hormone-like lipids stimulate the smooth muscles of the uterus to contract. From there, this initiates in the shedding of the blood and nutrient-rich endometrial lining, resulting in menstruation.
Menstrual Symptoms:
Contrary to popular belief, periods are not meant to be painful or symptomatic. The level of pain and symptoms a woman experiences with her period is highly associated with her systemic health. Menstrual symptoms are often as sign of increased inflammation levels, hormone imbalances, nutrient deficiencies, and more.
Understanding how to interpret these symptoms is key to utilizing the menstrual cycle as a vital sign and diagnostic tool.
Interpreting The Menstrual Cycle as a Vital Sign
Knowing the difference between a normal, healthy menstrual cycle and a dysfunctional, symptomatic cycle is going to help you to use the menstrual cycle as a vital sign and diagnostic tool.
A healthy period should ideally:
- Arrive around the same time every month. (21-35 day cycles are considered normal, however, 25-35 days may be more optimal for hormone health)
- Last an average of 3-7 days
- Have a total accumulated blood loss of 30-60 ml (or about 6-12 fully soaked regular tampons)
- Be a bright cranberry red in color with a thin, smooth consistency and zero to minimal clots.
- Have zero to minimal discomfort and pain (mild cramping may be normal)
- Not interfere with daily tasks and activities
Dysfunctions in menstrual health may appear as:
- Pre-menstrual mood swings or extreme mental/emotional discomfort
- Painful or debilitating cramps
- Pelvic pain outside of normal menstruation
- Extreme fatigue and/or brain fog (mild fatigue may be normal)
- Menstrual headaches & migraines
- Digestive issues: bloating, constipation, etc.
- Cycles shorter than 21 days or longer than 35 days
- Heavy bleeding or flooding (80 ml+ throughout the entire cycle)
- Brown, Dark Red or Purple Blood
- Blood clots larger than a quarter in size
- Irregular or skipped periods
- Missing periods for longer than 6 months
- Multiple days of spotting before and/or after menstruation
- Low or zero sex drive
- Vaginal dryness, vulvar sensitivity or pain with sexual intercourse
- Abnormal vaginal discharge
Although cycle symptoms may be common amongst menstruators, they are not biologically normal. Rather, they are symptoms of deeper underlying issues such as elevated inflammation, hormone imbalances, nutrient deficiencies, chronic stress, and more.
Charting the Menstrual Cycle as a Vital Sign
For some clients, it can be helpful to keep track of any symptoms they come across throughout their menstrual cycle.
This is important as observing cyclical patterns within the menstrual cycle can help you to recognize underlying issues and/or dysfunctions.
As an example, for some, chronic migraines around ovulation can be a sign of inflammation, excess estrogen, and histamine intolerance.
Utilizing information in this way allows us to get an inside look on their health. With that knowledge, we can provide them with strategic support for balancing their hormones and optimizing their health.
For an advanced level look at the menstrual cycle as a vital sign, one can chart certain biomarkers such as basal body temperatures and cervical mucus patterns. These biomarkers are commonly used when charting a cycle via a Fertility Awareness Based Method.
The Fertility Awareness Method is a method of non-hormonal fertility management that consists of the practice of observing and recording one’s fertile signs and fertile window, to successfully avoid or achieve pregnancy naturally.
Observing Cervical Mucus Patterns
It is normal to experience fluctuations in vaginal secretions throughout the menstrual cycle. Within the 5-6 days before ovulation, vaginal secretions may be more common.
In response to rising estrogen levels in the follicular phase, the cervix produces fertile-quality cervical mucus. This mucus may appear sticky, or tacky at first, but then evolves to become creamier, with more water concentration the closer to ovulation. Eventually, it can turn into a very slippery, egg-white quality of cervical mucus.
What About Vaginal Discharge?
The presence of fertile-quality cervical mucus is a sign of optimal fertility and is very different than vaginal discharge. Occasionally, women may observe fluid secretion outside of their fertile window. In this case, it would be considered vaginal discharge and not cervical mucus. This may also be an indicator of hormone imbalances, infection, or cervical dysplasia. Abnormal discharge should be examined further by a qualified medical professional.
Abnormal vaginal discharge that appears grey or greenish in color, has a foul odor, or is accompanied by itching or irritation is a sign of imbalance or infection and should also be examined by a qualified medical professional.
Observing Basal Body Temperatures
Keeping track of basal body temperatures is another way women can observe the health of their menstrual cycle.
To track basal body temperatures, your client will need a basal thermometer. This is a thermometer that records temperatures to at least 1/100th of a degree.
Instruct your clients to take their temperature first thing, at the same time every morning upon rising. They will want to ensure that they take their temperature before:
- moving or getting out of bed
- taking a sip of water
- looking at their phone
- engaging in conversation
- sexual activity
Temperature Patterns:
Temperatures in the follicular phase should ideally rest somewhere between 97.0 to 97.7 degrees Fahrenheit. Or, 36.11 to 36.5 degrees Celsius.
After ovulation occurs, they should see a sustained rise in temperature at least 1/10s of a degree (in Fahrenheit) above the previous 6 follicular temps. In celsius temps should be at least 0.05 degrees higher. Post-ovulatory temperatures may rise to 97.8 degrees Fahrenheit or 56.55 degrees Celsius and stay elevated until the next period arrives.
For those with troubles taking manual BBTs, technology such as the Tempdrop thermometer may be helpful in providing more consistent readings. Click here for a code redeemable for 10% off any Tempdrop thermometer.
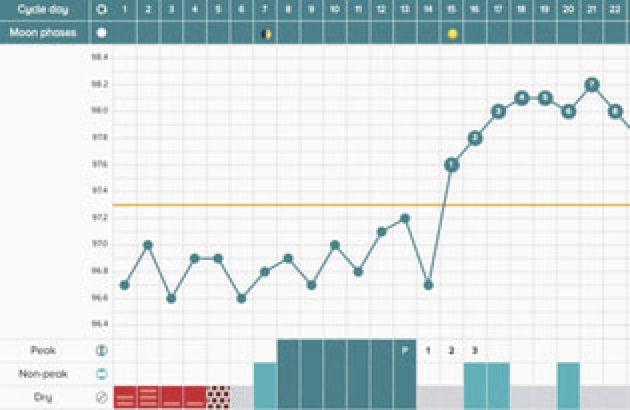
The Luteal Phase:
The thermal shift is a result of progesterone production in the luteal phase, which occurs only after ovulation. Progesterone has a thermogenic effect, stimulating thyroid hormone, increasing basal body temperatures. A sustained temperature rise is one way to confirm an ovulatory cycle.
If your client cannot determine if they experience a sustained temp rise, they may not be ovulating consistently. Or, they could just be taking their temperatures inaccurately. If you suspect the latter, recommend they visit a certified Fertility Awareness Educator. FAEs are trained professionals that teach clients to chart their cycles accurately.
Keeping track of basal body temperatures is a great way to confirm ovulation. However, it can also be used for assessing the status of thyroid health and function, adrenal health, and hormonal status.
Interpreting and Monitoring Progress
Keeping track of menstrual cycle symptoms, cervical mucus patterns, and basal body temperatures is a great way to use the menstrual cycle as a vital sign and diagnostic tool.
Menstrual cycle tracking can provide insight on
- ovulatory status
- sex hormone imbalances
- adrenal dysfunction
- thyroid dysfunction
- levels of inflammation
- and more
The tangible data that comes from cycle charting is absolutely invaluable. Cycle charting is an easy and free way that a woman can monitor her own health status and progress.
For example, the menstrual cycle can be heavily influenced by the quality of a woman’s nutrition, environment, sleep patterns, stress levels, and exercise routine. This means that through making simple, strategic nutrition and lifestyle adjustments, the menstrual cycle can change and improve over time. Through observing patterns in their menstrual cycle, women can keep track of their health progress.
The menstrual cycle is a woman’s internal report card – a vital sign – showing her precisely where she needs to make adjustments in order to experience a healthier, symptom-free cycle. A practitioners, we can use this tool in our practice to help our female clients achieve greater results.
Embracing The Menstrual Cycle as a Vital Sign
Now, more than ever, women need access to quality information about their reproductive health.
The more practitioners are familiar with this vital information, the more accessibility there is for women of this world. Through teaching women how to utilize their menstrual cycle as a vital sign and diagnostic tool, we have the power to instill change in our perspectives and approaches surrounding women’s health.
Do you want more information on how you can utilize the menstrual cycle as a tool in your practice? Be sure to check out our IAFHH Functional Hormone Specialist Certification Program.
This is our 16-week advanced continuing education program for practitioners. Within the program, we equip you with tools such as menstrual cycle charting and functional hormone testing in your practice. With these tools in place, you can help your clients achieve real and lasting results in their hormone health.

About the Author
Ashe Milkovic, NTP, IC-FHS, FBCS
Ashe is the founder and CEO of The International Association for Functional Hormone Health. She has a passion for spreading awareness about the power of functional nutrition for optimizing hormones & fertility, and her mission is to build community and safe space for other practitioners and aspiring learners to expand their knowledge and expertise in functional hormone health.
